


|
Health care as a part of public protection systems in the European countries Adam Kozierkiewicz Health policies, which are mainly the responsibility of the Member States, seek primarily to allocate available resources in order to achieve the best possible health outcomes. Health systems largely reflect health policies and arise from the interplay of many complex factors: demographic (population density and distribution, age structure, morbidity, mortality), ecological (climate and environment), cultural (behaviour, education, training), economic (industrial and occupational structure, level of development), social (public and private protection schemes), medical (medical practice), technological (availability of the most effective means) or legal (institutional practice). They are thus social constructs and how they are organised depends on how health services have developed and on the distinctive conditions in the various countries. There are as many health systems as there are countries and there have been many studies of the differences between them. We shall discuss them in terms of funding, system structure, medical practice and health care consumption. Funding reflects differences in the ability to mobilise resources In macro-economic terms, the level of health expenditure per capita reflects wealth of the country and the differences in the development of health systems. 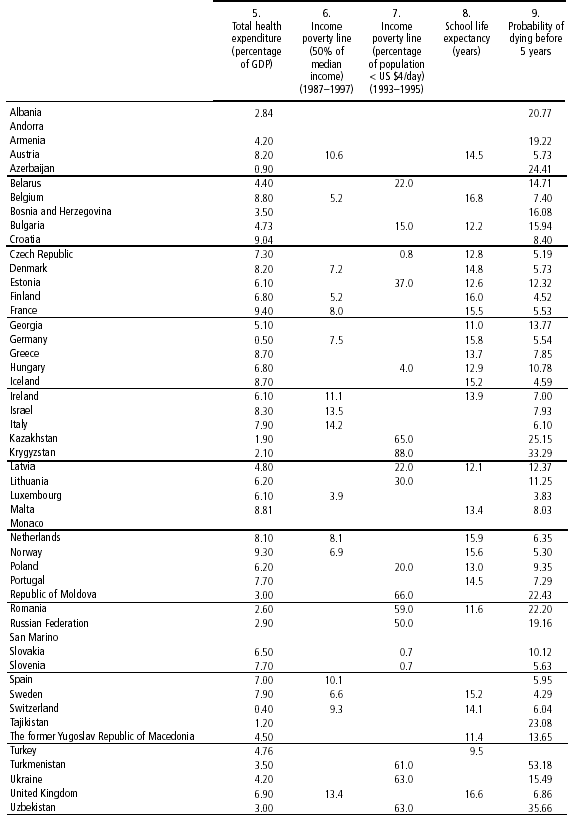 Purchasing Power Parities (PPPs) are currency conversion rates which express the purchasing powers of different currencies in terms of a common unit. In other words, when a given sum of money is converted into national currencies by means of PPPs, it will buy the same basket of goods and services in all countries. PPPs are thus currency conversion rates which eliminate the price differentials between countries. The variation shown in table above is largely explained by the relative wealth of the countries concerned. The OECD found that for every 100 dollars of difference in per capita GDP there is a difference of 10.50 dollars in per capita health expenditure. A 10% difference in per capita GDP corresponds to a 14% gap in health expenditure. Analysis of the data shows that differences in per capita GDP explain 77% of the variance in health spending. The link between GDP and health expenditure subsumes a complex set of relationships between different aspects of social and cultural life, economic structures, demography and variables specific to the health sector. The most striking feature of the last four decades has been the rapid growth of health spending in all industrialised countries, with the result that the proportion of gross domestic product (GDP) devoted to health has virtually doubled. The OECD established that the sharp rise in health expenditure in the last few decades was mainly caused by the increase in prices and intensity of use of medical services. The structure of health spending reveals a marked concentration of the cost of health care on a fairly small segment of the population. In some countries, 5% of the population have been found to account for 50% of health expenditure. On average, those over 65 account for four times as much as those of working age. If the health expenditure of the high-risk groups were not borne by the wider community, these persons would be unable to meet the cost of the treatment they require and it is very likely that their health, which in any case is poor and at great risk, would be further jeopardised. Socialised funding of health expenditure applies the principle of solidarity. This spreads the risks over the whole population, which generally contributes to the financing of the system according to income, through taxation or social security contributions. This is the only form of access to medical care which is predominantly intergenerational. On average, public expenditure on health, which mostly consists of spending on social protection, accounts for 70 to 85% of total health expenditure in the EU. Paradoxically, it is the low-GDP countries which have the lowest levels of socialised funding. The range extends from 91.8% for Luxembourg to 57.7% for Greece. Public expenditure as a percentage of total health expenditure Private expenditure as a percentage of total health expenditure (1990-2002) Two models and a wide range of variants of health care financing system The current forms of social protection date from the beginning of the industrial era. Industrial society is the context within which social protection has developed. The initial model was that of the mutual benefit societies of the 19th and the first half of the 20th century. In the course of the 20th century, public protection developed on the basis of two models: compulsory social insurance on the one hand and national health services on the other. These were also known as the Bismarckian and Beveridgian systems after their respective founding fathers. The first public social protection system came into being in Germany. Chancellor von Bismarck achieved his aim of defusing social tensions by introducing a social insurance plan in 1880, organising protection against social risks through insurance. His main innovation was to institutionalise the principle of making insurance compulsory for both workers and employers and to relate contributions to earned income. The first law instituting the principle of compulsory social insurance was passed in Germany in 1881 and related to sickness insurance. It was based on the practice applied at the time by Germany's 10 000 sickness funds. When the United Kingdom had to reorganise its hospital system during the Second World War, it introduced a different philosophy of protection against the risk of illness: the national health service. The National Health Service model was devised by a task force chaired by Lord Beveridge and the service was later set up in 1948 on the basis of four essential principles:
All European countries have based the structure and funding of their health systems on one of these two approaches. Initially, the Bismarckian model spread among the most highly industrialised countries in the first half of the 20th century. Protection was initially limited to wage-earners and was gradually extended to the whole population, except in Germany and the Netherlands, where certain groups (mainly those earning above a certain income level) can or must obtain private insurance. In the Northern European countries, various reforms led to the establishment of health systems in the 1960s. These were partly inspired by British experience but at the same time rested on the principles of social insurance and local management of the system. This combination is known as the Nordic model. In the Mediterranean countries, the radical political changes of the 1970s led to national health systems on the Beveridgian model, ensuring a universal right to health care. It is always risky to construct typologies and classify the various forms of social protection, which are the result of the historical and institutional development of the country concerned. However, it is generally accepted that the Member States of the European Union can be grouped as follows:  Without going into the details of each system, this typology highlights the guiding principles underlying the collectively funded systems for ensuring access to health care.Social insurance systems generally offer category-based protection. In Belgium, there are two separate regimes: the first covering the whole population apart from the self-employed and the second covering only the self-employed and only for the major risks. In France, there are three regimes: for employed workers and civil servants, for the self-employed and for farmers. In Germany, those with incomes above a certain level are not subject to compulsory insurance. In the Netherlands, those with incomes above a certain level are excluded from the public system. These systems are managed by the social partners. In the countries with compulsory social insurance, two systems for meeting medical costs may be Distinguished:
In the countries with national health services, delivery of health care and ensuring its access are integrated into one single organisation. It is the state, whether in centralised or decentralised mode, which satisfies citizens' demand for care by ensuring access to health services. Generally, the patient has no out of pocket payments to make except for any standard charges. Coverage is usually universal. However, in some countries there are echoes of an earlier category-based system. This is the case e.g. in Denmark (service provider freely chosen by the patient) and in Ireland (free treatment or partial payment depending on income). Most of these countries fund their systems from taxes (United Kingdom, Ireland, Denmark, Finland, Sweden, Norway, Portugal). Despite these fundamental differences, the position of certain countries within the typology has changed considerably over the last twenty years under the pressure of measures to contain health spending. Each model has thus incorporated management and funding techniques based on the other. The health care systems have thus tended to converge towards hybrid systems. The main reason for these convergent trends is that the systems are facing the same challenges. The first is the sharp rise in health expenditure resulting from several factors such as rapid progress in developing new and costly medical techniques, the high cost of new medicines placed on the market and the medicalisation of social problems. Secondly, the slowdown in economic growth, efforts to ensure sound public finances and the desire to reduce labour costs in order to create employment are exerting greater pressure on collective funding capacities. Finally, the demographic ageing of the populations is weighing increasingly on collective provision for medical costs and especially on the investment required to tackle the new needs to which this process gives rise. Wide discrepancies in medical practice The diversity of the EU Member States' health care and care access systems is apparent on many other levels: health outcomes, medical practice, forms of health care consumption, etc. Two reliable indicators are life expectancy at birth and the infant mortality rate. Their divergence, which is sometimes considerable, reveals substantial differences from which some citizens will benefit and others unfortunately suffer. 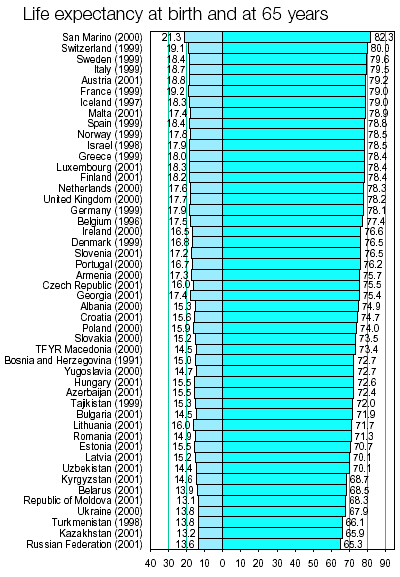 Among the EEA countries, the widest gap in life expectancy at birth is 4.1 years for women (France/Denmark) and 5.5 years for men (Iceland/Portugal). The 1995 infant mortality rate was 8.2 deaths per 1000 live births in Greece, and only 4, less than half as high, in Finland. 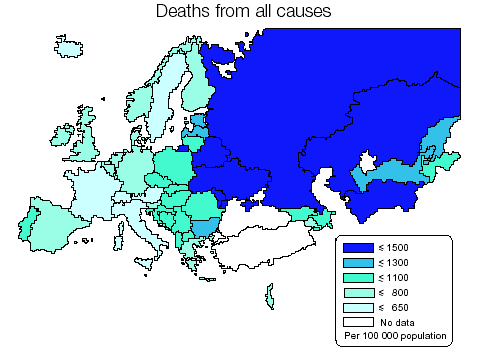 The above map shows the rates per 100 000 head of population for the main causes of death. The fact that the figures diverge - sometimes considerably - within the EEA raises many questions as to the data collected, the factors determining the onset of disease (quality of life, diet, working conditions, environment, etc.) and the treatment provided, as well as prevention. Cardiovascular diseases kill four times as many people in Portugal as in France. Myocardial infarction causes four times as many deaths in Ireland as in Luxembourg. Respiratory diseases lead to four times as many fatalities in the United Kingdom as in Austria. 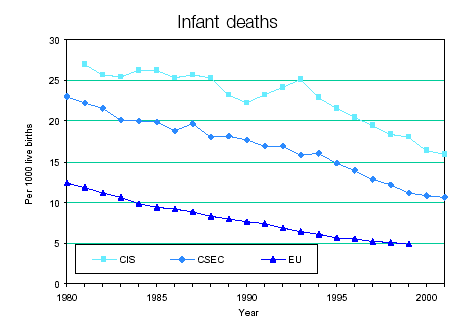 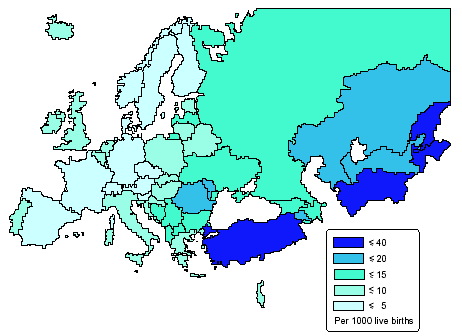 Another aspect of diversity in the health sector, both between countries and within each country, is the persistence of social inequalities. These are apparent as inequalities in consumption and treatment. French research is very revealing. It shows, for example, that the death rates for men aged 25 to 64 and employed as blue or white-collar workers were three times as high as those for the higher professions (for the period 1989-1994). Ten years before, this excess mortality factor was 2.5. In other terms, it is the social categories with the lowest death rates which benefit most from the general increase in life expectancy. In France, the life expectancy of male manual workers at the age of 35 is 8.8 years less than that of primary school teachers and 7.3 years less than that of senior managers and practitioners of the liberal professions. Mortality rates differ from birth and are probably linked with the state of health of the parents and with circumstances and social conditions during pregnancy. Analysis of the causes of death reveals mortality differentials depending on social class in both France and the United Kingdom. These are particularly marked for deaths due to tuberculosis, cirrhosis, lung disease, accidents and certain cancers. Recent French statistics illustrate mortality differences between social classes for most diseases (premature death rate from alcoholism and cancers of the upper aerodigestive tract ten times as high for white/blue-collar workers as for managers and the liberal professions, four times as high for lung cancer, three times for cerebrovascular and hypertensive diseases, traffic accidents, suicide). DESPLANQUES G. ibid. demonstrated the link between mortality and level of education. Male mortality is inversely proportional to the educational level. He also observes that death rates are higher for the unemployed in all social categories and as one descends the social scale this excess mortality increases. Health care consumption profiles differ according to social category. The less-advantaged tend to consult general practitioners and to be treated more in hospital. The more affluent consume more specialist consultations, dental care, medicines, whether prescribed or otherwise, blood tests, physiotherapy and home nursing. For managers and white-collar workers, differences in the frequency of consultation of doctors and dentists increased during recent decades. Social inequalities in health outcomes are explained firstly by disparities in social conditions and the related cultural and behavioural differences. Another explanatory factor is access to treatment. The most disadvantaged households tend to postpone or renounce to certain types of care because health spending represents a relatively high proportion of their budget. This leads to the development of serious illnesses. The poorest strata of the population end up more often in hospital and spend more time there than the better-off. Various studies have identified behaviour patterns which endanger health. These are more common among the less well-off. Three examples are smoking, diet and physical activity. The percentage of smokers is higher among the lower classes. However, the link between smoking and class varies greatly from country to country. It is very strong in France, Italy and Norway and very weak in the United Kingdom. In Spain, the well-off tend to smoke more. The same applies to alcohol consumption. The disadvantaged tend to have a less well-balanced diet. Fat consumption has been found to be twice as high. Poor diet increases the risks of diabetes, obesity and anaemia and reduces resistance to disease. Finally, managers average twice as much sporting activity as manual workers. Inter-country and intra-country comparisons reveal considerable variation in the frequency of a particular medical operation or the consumption of medicines or treatments for the same illness. The number of pacemakers fitted per million head of population16 is 600 in Belgium, 450 in France and the former West Germany, 300 in Denmark and a little over 200 in the United Kingdom. The index for ambulatory pharmaceuticals consumption per head of population is 180 in France, 140 in Italy, 100 in Belgium, 40 in the Netherlands and under 35 in Denmark1. The number of patients treated for kidney failure is 400 per million in Belgium, 300 in Italy and France and 250 in Greece. In Belgium, the number of days spent in psychiatric hospitals per 1000 inhabitants varies greatly from region to region: 346 days in Brussels, 587 in Wallonia and 861 in Flanders. A recent study on hysterectomy provided further confirmation of the many observations of uneven health practice, with large variations from country to country and from region to region within Belgium. The risk of undergoing the operation is an inverse function of the patient's educational level and income. There are substantial variations in the technique employed (abdominal or vaginal surgery with or without laparoscopy). The main explanatory factors are the training and opinion of the surgeon and the age of the patient. Cost and length of stay depend on the hospital concerned. The indicators of health outcomes and consumption of health care reveal large differences between the countries. While some part is played by population-related factors (demographic composition, differential morbidity, differences in unhealthy lifestyles), little is yet known about their importance. Other factors which operate additionally or in conjunction relate to the supply of health care (organisation, funding, prescribers' attitudes) and more general factors which may be cultural (attitude to health, illness etc.), economic and political (organisation of social protection). Cost containment and related reforms The diversity of social protection systems has spawned a host of cost containment mechanisms. In many countries, policy-makers have concentrated on controlling supply, using a wide range of complex and ingenious measures, which fall into four categories:
Generally speaking, states which are forced to stabilise the level of health expenditure in order to curb public funding of health care seek to impose overall and sectoral budgets and regulate growth of public spending. Such measures tend to shift more of the burden of health care funding on to households by reducing cover or failing to keep pace with rising costs. Today, budgeting and cost sharing by patients apply in virtually all systems. Higher patient contributions are intended to discourage or limit demand. However, to reduce the negative impact of such policies on access to treatment and to make them more acceptable, certain categories, such as low-income groups and/or patients suffering from serious or chronic illnesses, are entirely or partly exempted. Cost containment is part of the efforts to achieve a more rational allocation of resources according to needs. Since the mid-1980s, ambitious reform projects have sought to attain this rationality/efficiency by introducing competition among the actors in the health care sector. As patients and/or insureds are given "consumer's freedom of choice", providers and/or insurers (purchasers of care), being alloted a prospective budget are incited to adopt an accountable approach in providing quality care at minimum cost. Even if this approach does not seem to have much effect in curtailing expenditure, the reforms which it drives are changing the health care landscape, leading to mergers and reinforcing the trend towards regionalisation. The quest for rationalisation is also apparent in the concept of "evidence based medicine", i.e. reimbursement of the cost of treating an illness is determined on the basis of the diagnostic and therapeutic methods whose effectiveness has been demonstrated. A benchmark is thus established on the basis of the current state of knowledge and the treatment given is compared with this benchmark. However, these methods of defining "quality standards" cannot be applied to all medical practice. In particular, they are inappropriate for palliative care. Since the cost control measures strike against an incompressible mass of highly concentrated costs, they yield only modest savings and the risk of care rationing is therefore increased. Specific examples are the development of waiting lists or refusal to provide particular kinds of treatment to patients above a certain age. Overall, the reforms pursued over the last twenty years have concentrated primarily on restricting supply and less on adjusting demand. In a second phase, they have extended to the areas of responsibility of the parties concerned. |
